10 MAY 2026
Could Skin-Level Spinal Cord Stimulation Help Calm Autonomic Dysreflexia After SCI?
A new UBC thesis study in rats suggests that transcutaneous spinal cord stimulation may reduce autonomic dysreflexia by activating the spinal cord's own inhibitory 'braking system', helping quiet the overactive reflexes that drive dangerous blood pressure spikes after high-level SCI.
Deep Dive
Autonomic dysreflexia, often shortened to AD, is one of the most frightening secondary complications of spinal cord injury.
It can come on fast. A blocked catheter, full bladder, bowel problem, skin irritation, pressure sore, tight clothing, or another trigger below the injury level can cause a sudden spike in blood pressure. For people with cervical or upper thoracic SCI, this can mean pounding headache, sweating, flushing, goosebumps, anxiety, chest tightness, slow heart rate, and a real medical emergency.
This story is especially relevant for people who live with severe or repeated AD. The study does not offer an immediate home treatment, but it helps explain why non-invasive spinal cord stimulation could become a useful tool for reducing AD in the future.
The research comes from a 2026 University of British Columbia thesis by Hari Prasad Joshi, supervised by Professor Andrei Krassioukov, a leading researcher in autonomic dysfunction after spinal cord injury.
Author(s):
Hari Prasad Joshi. Supervisory and examining contributors included Andrei V. Krassioukov, Ismail Laher, Rahul Sachdeva, Soshi Samejima, Alexander G. Rabchevsky, and Keith E. Tansey.
Source:
University of British Columbia, Faculty of Graduate and Postdoctoral Studies, Experimental Medicine. Thesis title: "Unraveling the Mechanism of Transcutaneous Spinal Cord Stimulation in Mitigating Autonomic Dysreflexia in Experimental Spinal Cord Injury."
What AD is, in plain English
The autonomic nervous system controls automatic jobs: blood pressure, heart rate, sweating, blood vessel tightening, bladder, bowel, temperature regulation, and more.
After a high spinal cord injury, the brain can lose proper control over many of these automatic circuits below the injury. The lower body can still send alarm signals into the spinal cord, but the brain's calming control cannot always get back down properly.
A useful analogy is a smoke alarm that is wired to a sprinkler system but no longer connected to the control room. Something small sets off the alarm, the sprinkler system overreacts, and nobody upstairs can easily switch it off.
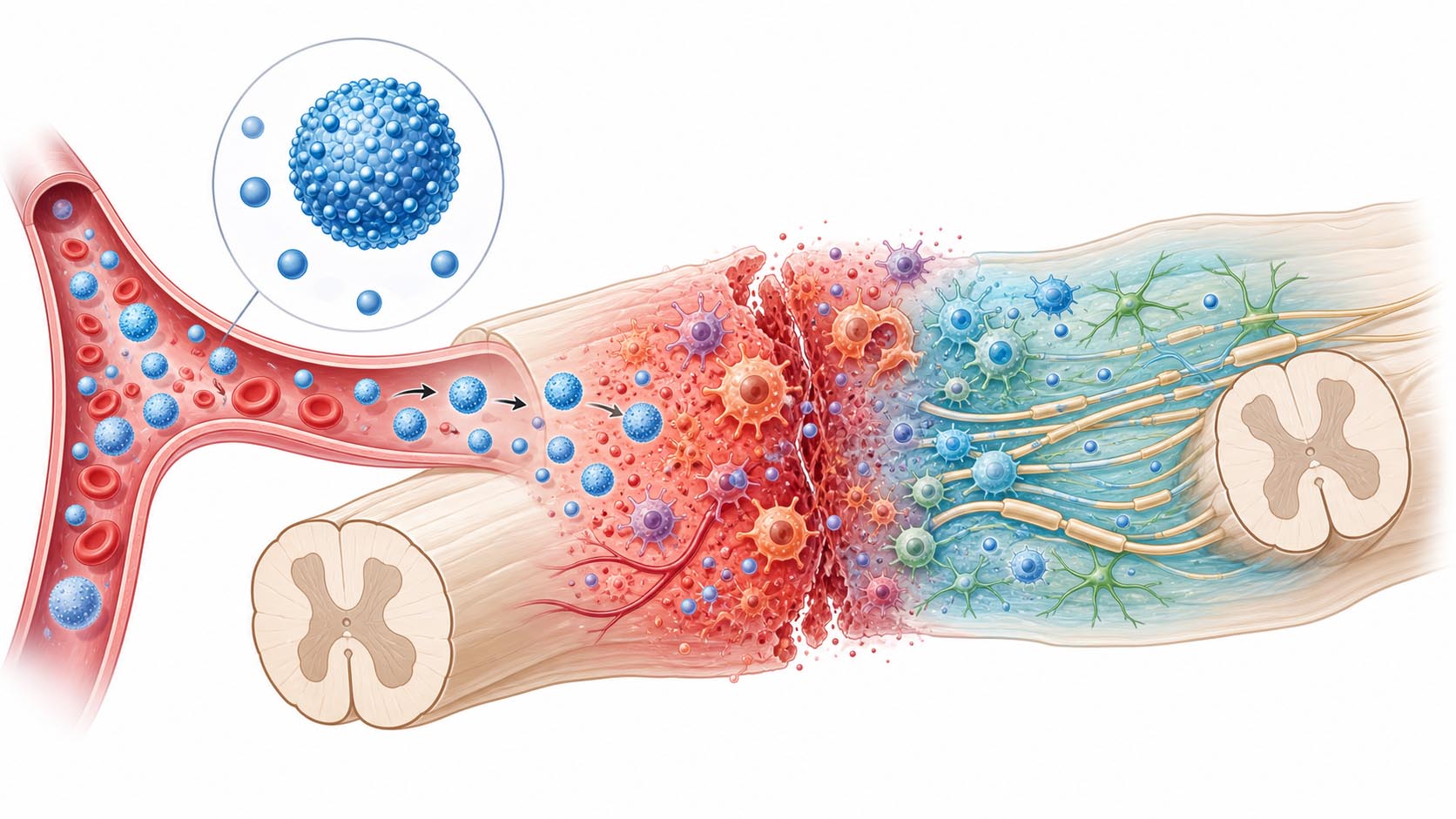
In AD, a trigger below the injury level can cause blood vessels below the injury to clamp down hard. Blood pressure rises quickly. The brain senses the high pressure and tries to slow the heart, but it cannot fully relax the blood vessels below the injury because the spinal cord pathway is interrupted.
That is why AD is not just uncomfortable. It can be dangerous.
The idea: use stimulation to restore the spinal cord's brake
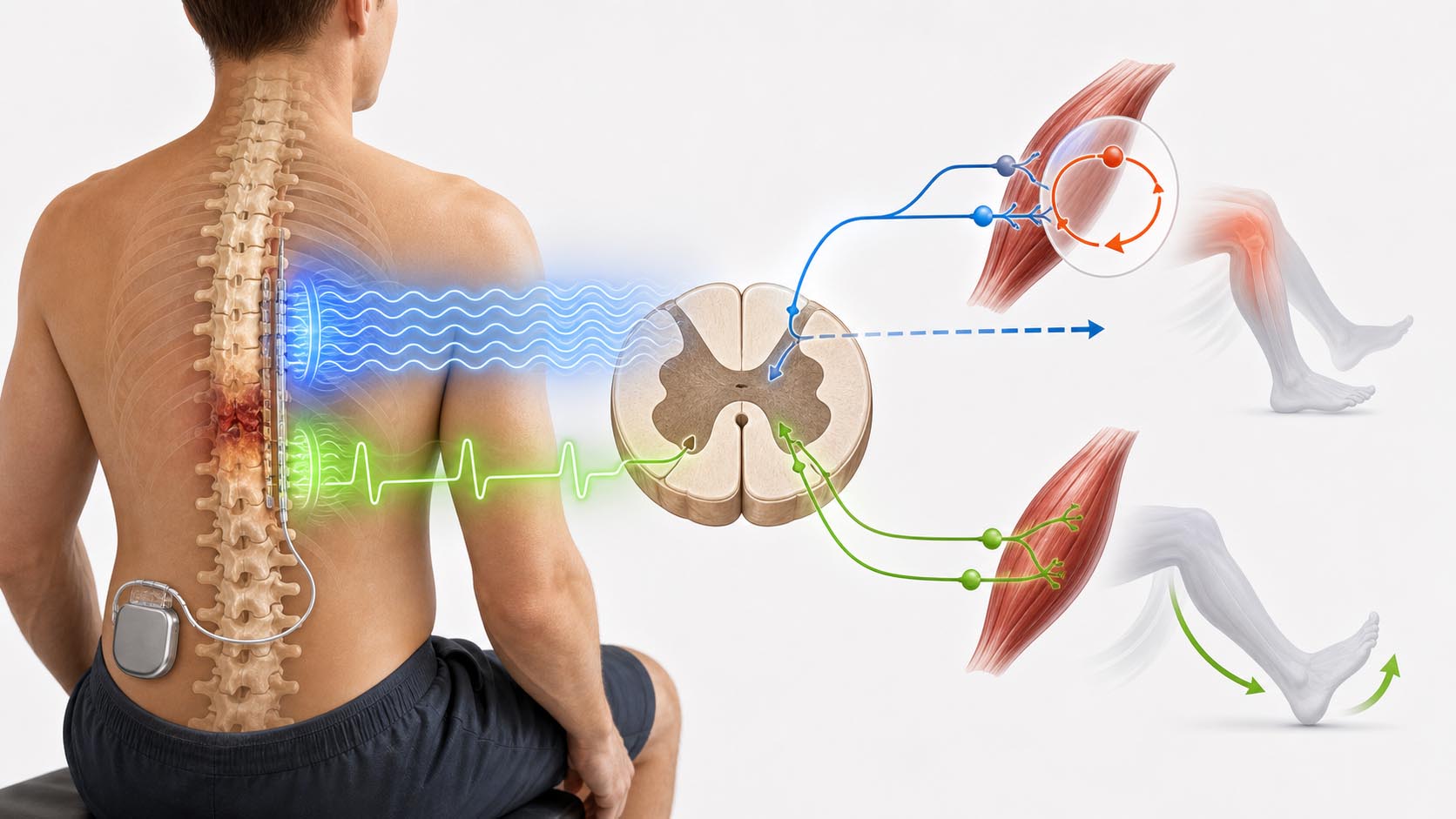
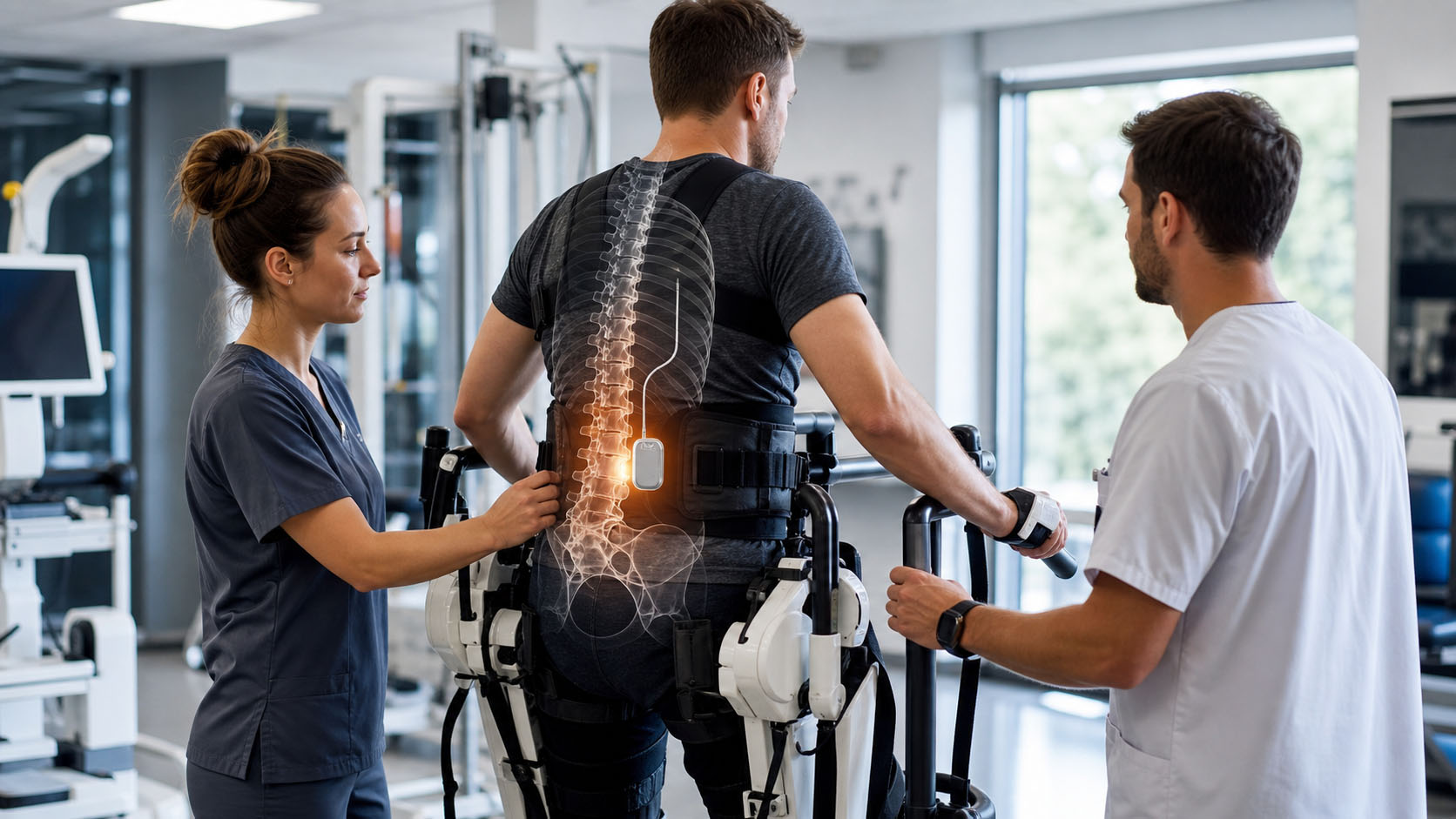
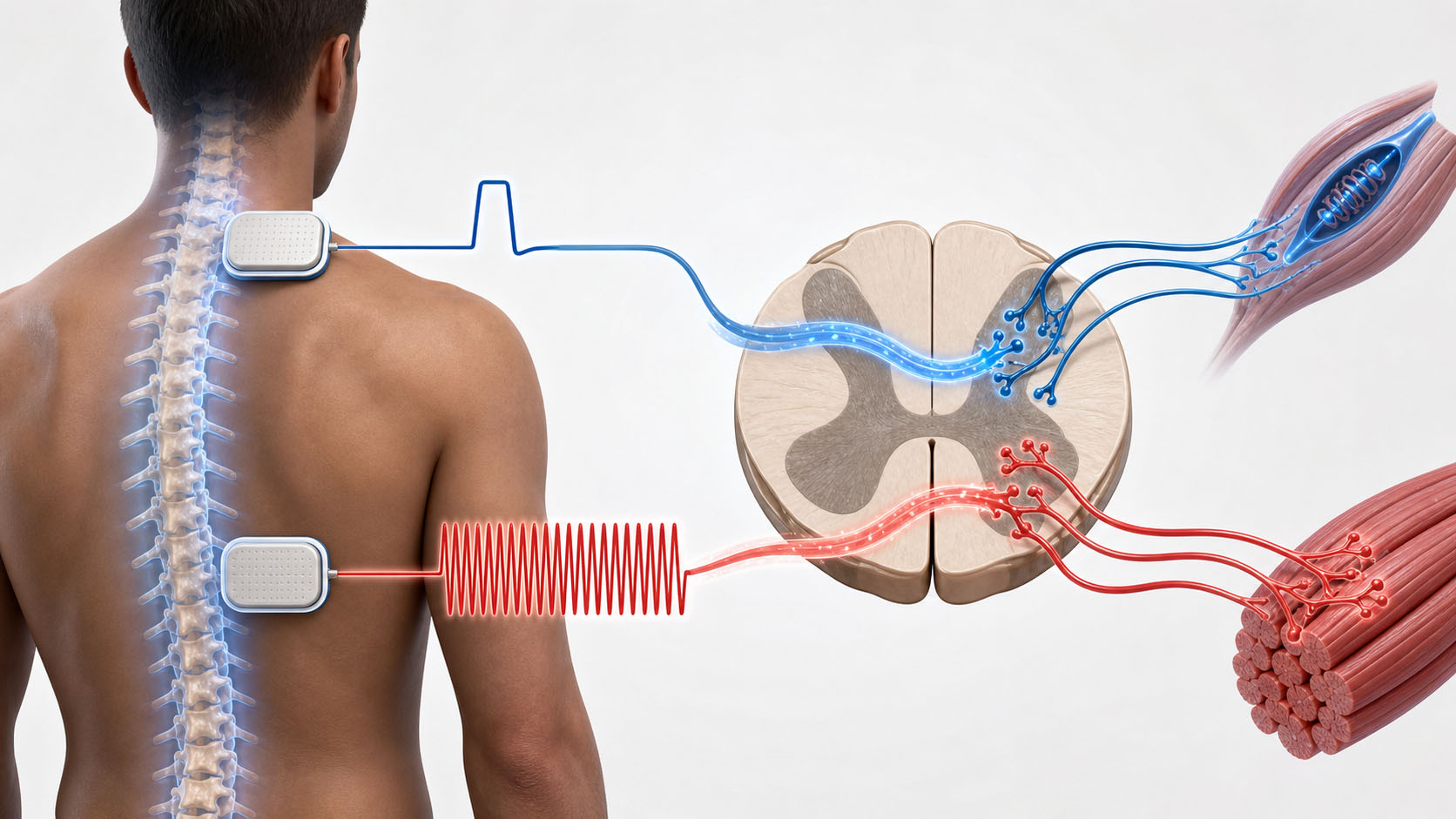
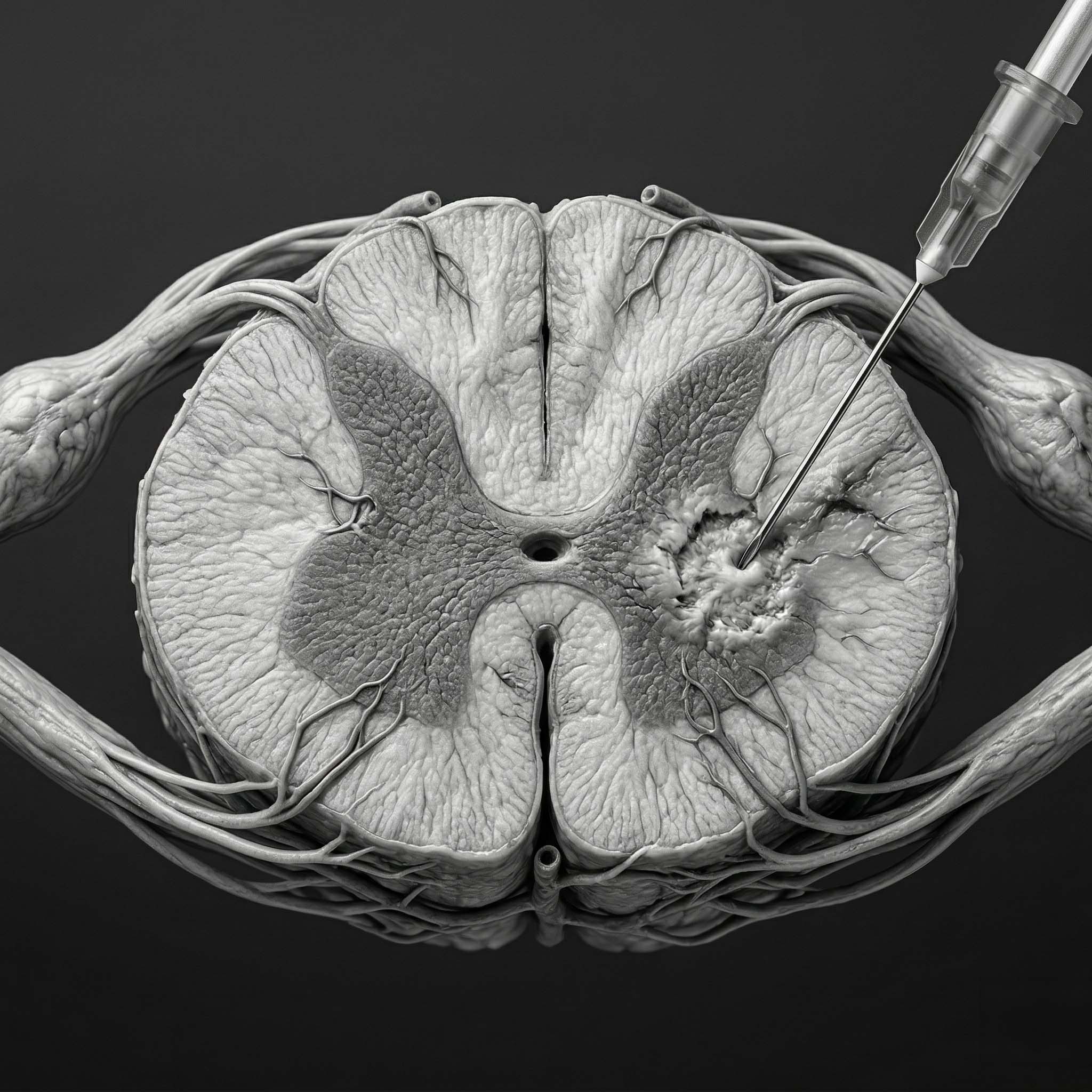
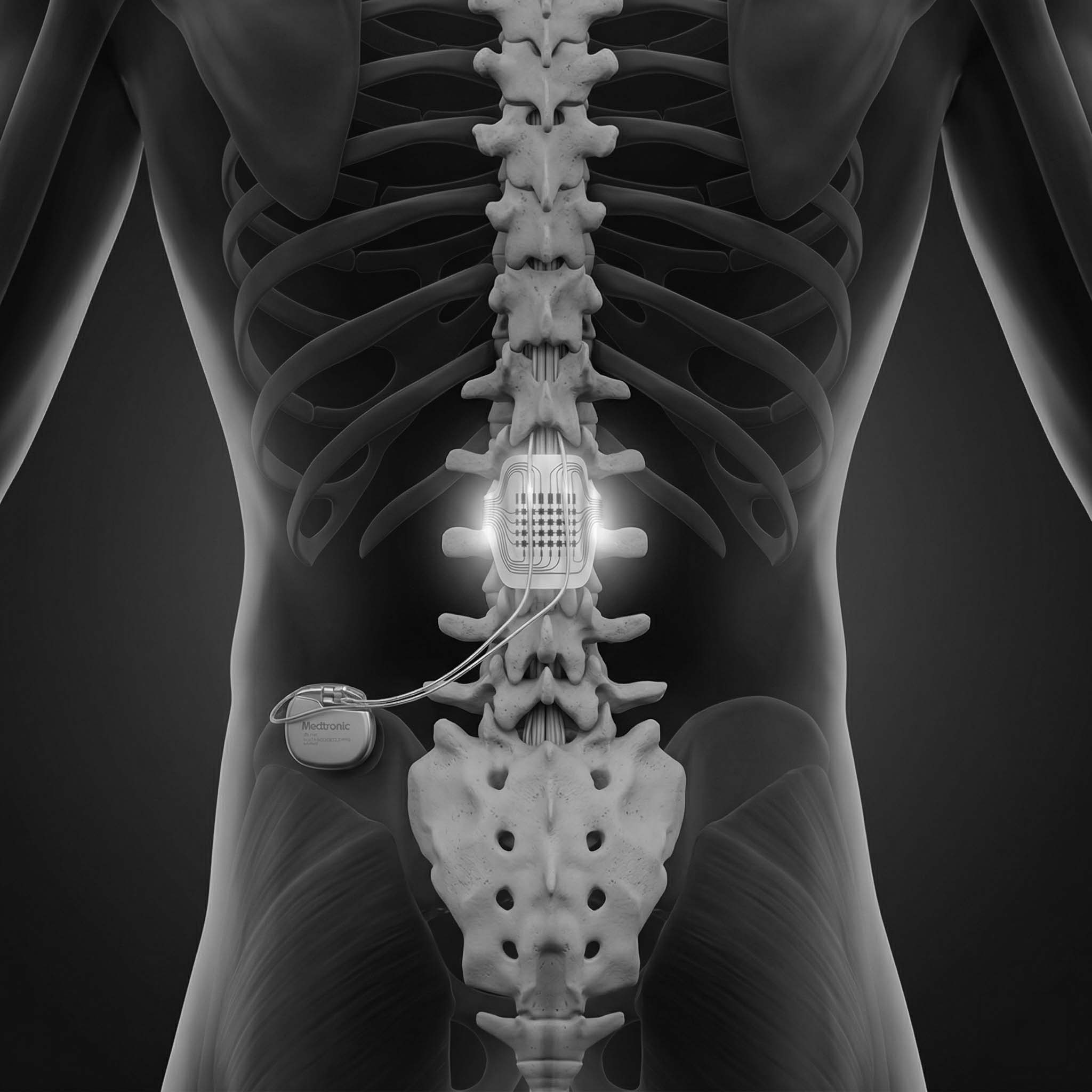
The study looked at transcutaneous spinal cord stimulation, or tSCS.
"Transcutaneous" means through the skin. Unlike implanted epidural stimulation, tSCS uses surface electrodes placed on the skin over the spine. The goal is to send electrical pulses into spinal circuits without surgery.
In this rat study, stimulation was delivered over the T7 spinal segment using 30 Hz pulses for 60 minutes. The model involved a high thoracic T3 spinal cord contusion injury. Six weeks later, the researchers triggered AD-like spinal activity using colorectal distension, a standard experimental model because bowel or rectal distension is a common real-world AD trigger.
The big question was not simply "does stimulation reduce AD?" Previous work had already suggested tSCS can reduce AD. This study asked a deeper question: how might it work inside the spinal cord?
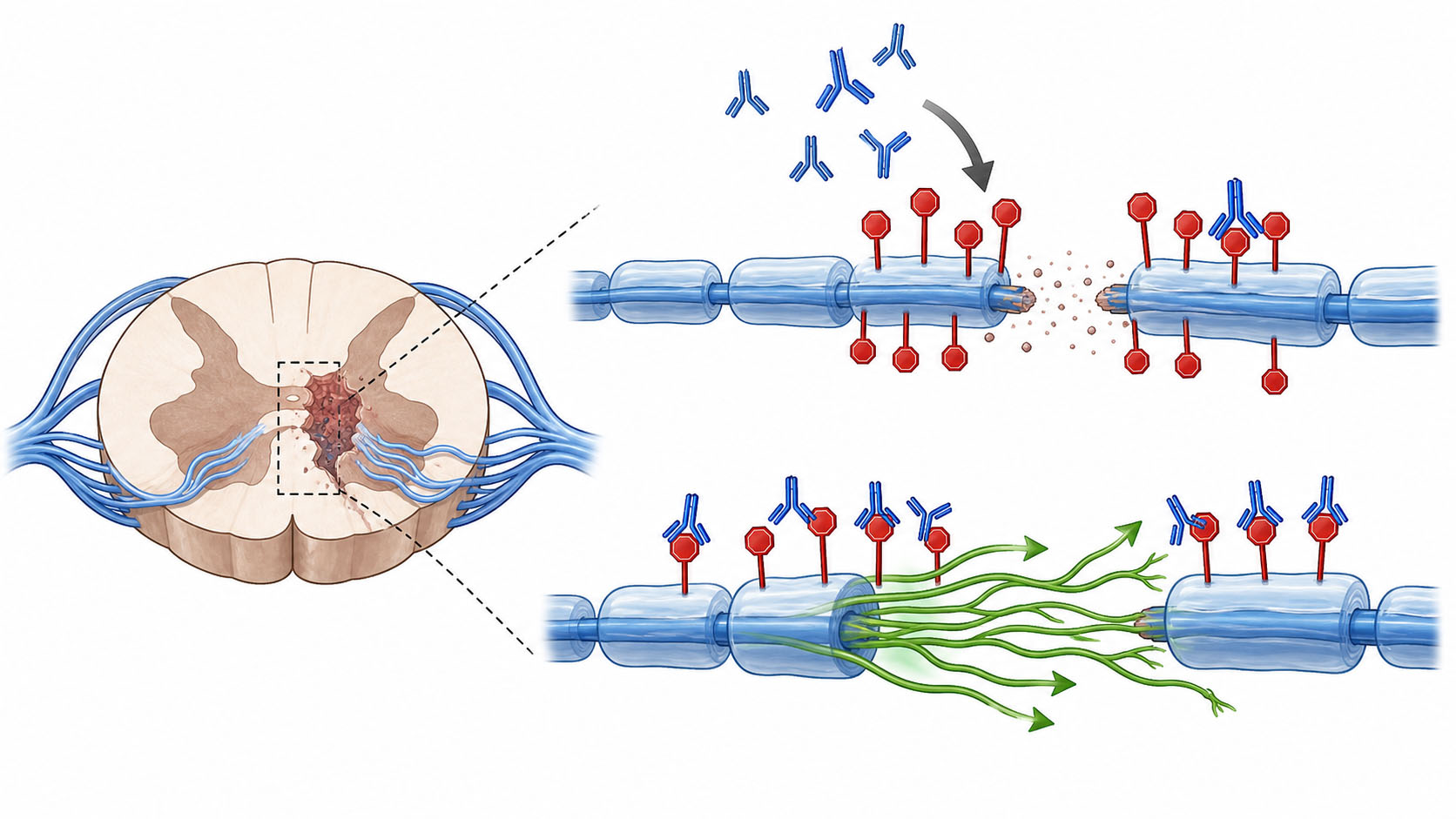
The spinal cord after SCI can become too excitable
After SCI, the spinal cord below the injury is not silent. It can rewire itself.
Some rewiring may be helpful. But some becomes maladaptive, meaning it makes symptoms worse. In AD, sensory signals from the bowel, bladder, skin, or other areas below the injury can over-activate spinal circuits that control sympathetic output. Sympathetic output is the "fight or flight" side of the autonomic system, and when it overfires it can drive blood pressure dangerously high.
The key cells in this process include sympathetic preganglionic neurons, or SPNs. These are spinal neurons that help send commands to the sympathetic nervous system. When they become overactive after a trigger, they can contribute to the blood pressure surge of AD.
The thesis found that colorectal distension strongly activated spinal neurons and SPNs after SCI. That fits the AD pattern: a visceral trigger below the injury sends a powerful signal into overexcitable spinal autonomic circuits.
What stimulation changed
When tSCS was applied at the same time as colorectal distension, the overactivation was reduced.
The researchers used markers such as c-Fos to identify activated neurons. They found that the CRD trigger increased neuronal activation across multiple spinal segments. But when CRD was paired with tSCS, that activation was significantly reduced compared with CRD alone.
Most importantly, tSCS reduced activation of the sympathetic preganglionic neurons involved in driving autonomic output.
At the same time, tSCS increased activation of inhibitory spinal interneurons. These are local spinal neurons that help quiet other neurons. The study focused on inhibitory systems involving GABA and glycine, two chemical messengers that act like brakes in the nervous system.
In plain English: stimulation appeared to turn down the overactive alarm circuit and turn up the spinal cord's braking system.
Why GABA and glycine matter
GABA and glycine are inhibitory signals. They help stop nerve circuits from firing too strongly.
In everyday terms, if excitatory signals are the accelerator, inhibitory signals are the brake. AD may partly happen when the accelerator gets stuck and the brake is too weak. This study suggests tSCS may help press the brake at the spinal level.
That does not mean tSCS "cures" AD. It means stimulation may change the balance inside the spinal cord so that bowel or bladder signals are less likely to explode into a dangerous sympathetic reflex.
Why this matters for people who live with AD
For someone who gets severe AD, the practical goal is not abstract. It is fewer dangerous spikes, less fear around bladder and bowel routines, better sleep, less strain on the heart and brain, and more confidence that the body will not suddenly swing into crisis.
Repeated AD episodes may also matter for long-term health. Blood pressure instability after SCI is linked to cardiovascular and cerebrovascular risk, and researchers increasingly worry that repeated highs and lows could affect brain blood flow and cognition over time.
A non-invasive stimulation method would be especially valuable because it could potentially be used repeatedly, adjusted to the individual, and delivered without implanted surgery.
What this study does not prove yet
This was an experimental rat study, not a human clinical trial.
The researchers studied spinal cord tissue and neuronal activation patterns after stimulation. That gives important mechanism information, but it does not by itself prove that the same stimulation settings will safely and reliably prevent AD in people.
The study also used a specific injury model, timing, stimulation site, and stimulation parameters. Human SCI is more varied: injury level, completeness, time since injury, bladder and bowel routines, medications, spasticity, pain, skin triggers, and cardiovascular health all differ between people.
So the fair conclusion is careful but encouraging: tSCS appears to recruit inhibitory spinal circuits that can dampen AD-related sympathetic activation in an animal model. That gives researchers a stronger reason to test and refine tSCS for AD in people with SCI.
Why this matters in SCI
AD is often treated as a management problem: find the trigger, sit upright, loosen clothing, empty the bladder or bowel, check the skin, monitor blood pressure, and use medication if needed. That emergency approach remains essential.
But this research points toward something more preventive: changing the spinal cord circuits that make AD so explosive in the first place.
If future human studies confirm the effect, tSCS could become part of autonomic rehabilitation. Not just rehabilitation for muscles or walking, but rehabilitation for blood pressure control and internal body stability.
For people living with severe AD, that would be a meaningful goal.
Reader Q&A
Could I use a home electrical stimulator to treat AD now?
No. This should not be tried independently. AD can be dangerous, and spinal stimulation settings, electrode placement, and patient selection need clinical testing. Anyone having AD episodes should follow their medical AD plan and speak with their SCI clinician.
Is this only relevant to bowel-triggered AD?
The experiment used colorectal distension because bowel and rectal distension are reliable AD triggers in research and real life. The mechanism may also matter for bladder or other triggers, but that needs direct testing.
Why is this exciting if it was only in rats?
Because it explains a possible mechanism. It suggests tSCS may work by activating inhibitory spinal circuits, not just by generally "stimulating the spine". Mechanism matters because it helps researchers choose better stimulation locations, strengths, and timing for future human trials.